Executive Summary
This EHR implementation checklist outlines the key planning, operational, and technical steps clinics should complete before an electronic health record system goes live. Successful implementation requires more than installing software because it involves changes to clinical workflows, staff responsibilities, and daily operations. Clinics that follow a structured approach are better prepared to reduce disruption, support staff adoption, and maintain stable revenue cycle performance. In this guide, we walk through the phases organizations should complete to prepare for go live and improve long term outcomes.
Key Takeaways
- 1. Executive Summary
- 2. Key Takeaways
- 3. Why Clinics Implement EHR Systems During Summer
- 4. EHR Implementation Timeline At A Glance
- 5. Strategic Planning Using an EHR Implementation Checklist
- 6. Using an EHR Implementation Checklist for Vendor Selection
- 7. Workflow Mapping And Data Migration
- 8. Staff Training And Change Management
- 9. Using an EHR Implementation Checklist for Go-Live Preparation
- 10. Using an EHR Implementation Checklist for Post-Implementation Optimization
- 11. Conclusion And Next Steps
- 12. Ready to Talk?
- 13. Further Reading
- 14. Related Articles
Why Clinics Implement EHR Systems During Summer
Many clinics use an EHR implementation checklist to plan go live during the summer because it allows more flexibility and reduces operational risk. Summer months often provide lower patient volumes, which gives staff more time to focus on training and workflow changes. This timing also aligns with healthcare planning cycles and approved budgets, which makes it easier to move forward with EHR implementation. Clinics that follow a structured EHR implementation checklist and begin preparation in Q2 are more likely to complete workflow design, data migration, and testing without delays. This approach supports a smoother go live and better long term adoption.
EHR Implementation Checklist And Seasonal Planning Cycles
Healthcare organizations often begin using an EHR implementation checklist after completing strategic planning early in the year. Leadership teams define priorities, approve technology investments, and align on EHR implementation goals. This early planning phase ensures that clinics can move into vendor selection and workflow design with clear direction.
EHR Implementation Checklist And Lower Patient Volume
Lower patient volumes during summer months support a more effective EHR implementation checklist by giving staff time to participate in training and system testing. Clinics can adjust schedules and reduce workload pressure, which helps improve learning and adoption of the new EHR system.
EHR Implementation Checklist And Budget Timing
An EHR implementation checklist is often activated once budgets are approved in Q1 or early Q2. This allows organizations to allocate funding for software, hardware, and implementation services. Clinics can move forward with vendor selection and begin structured implementation planning with fewer financial delays.
EHR Implementation Checklist And Q2 Preparation
Starting an EHR implementation checklist in Q2 gives clinics enough time to complete critical steps before go live. These steps include workflow mapping, data migration planning, staff training, and system testing. Organizations that follow a structured checklist reduce the risk of rushed implementation and improve overall outcomes.
For organizations that need structured guidance during this phase, our EHR Consulting Services help clinics manage timelines, coordinate vendors, and execute each step of the EHR implementation checklist with greater consistency and control.
EHR Implementation Timeline At A Glance
A structured EHR implementation checklist depends on a clear and realistic timeline. Clinics that follow a defined timeline are better able to manage resources, coordinate vendors, and complete each phase of implementation without delays. Breaking the process into phases allows organizations to focus on planning, workflow design, training, and testing at the right time. A well organized EHR implementation checklist reduces risk and helps ensure a smooth and controlled go live.
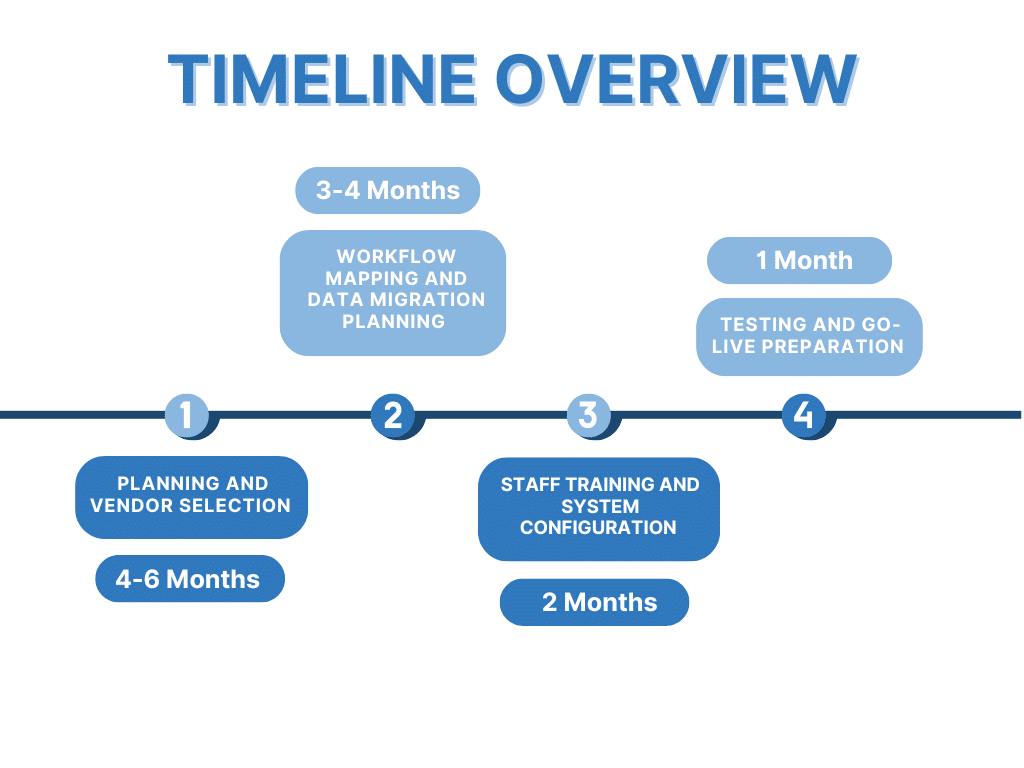
EHR Implementation Checklist 4 To 6 Months Before Go Live
The first phase of an EHR implementation checklist focuses on planning and vendor selection. Clinics define goals, evaluate vendors, and establish project governance. This stage sets the foundation for the entire implementation and ensures that the selected system aligns with clinical and operational needs.
EHR Implementation Checklist 3 To 4 Months Before Go Live
At this stage, the EHR implementation checklist shifts to workflow mapping and data migration planning. Clinics document current workflows, identify inefficiencies, and begin designing how processes will function in the new system. Data migration strategies are also defined to ensure accurate transfer of patient information.
EHR Implementation Checklist 2 Months Before Go Live
Two months before go live, the EHR implementation checklist focuses on staff training and system configuration. Clinics begin role based training, develop documentation, and prepare staff to use the system in real scenarios. This phase is critical for building confidence and supporting adoption.
EHR Implementation Checklist 1 Month Before Go Live
In the final phase, the EHR implementation checklist centers on testing and operational readiness. Clinics conduct end to end testing, validate workflows, and confirm that all integrations are working correctly. Teams also prepare for go live by adjusting schedules and confirming support resources.
Strategic Planning Using an EHR Implementation Checklist
A successful EHR implementation checklist begins with strong strategic planning. Clinics that invest time in planning are better prepared to manage timelines, coordinate teams, and avoid costly delays. This phase of the EHR implementation checklist focuses on defining goals, assigning leadership, and preparing the organization for system wide change. Clear planning creates alignment across clinical, operational, and technical teams and sets the foundation for a smooth implementation.
EHR Implementation Checklist Define Implementation Goals
An EHR implementation checklist should begin with clearly defined goals that guide the entire project. Clinics often focus on improving clinical documentation, strengthening revenue cycle performance, supporting regulatory compliance, and expanding reporting capabilities. Clear goals help ensure that system configuration and workflow design align with long term organizational priorities. Clinics looking to improve system performance after go live can also explore practical optimization strategies in our insight on NextGen EHR tips and tricks to boost patient outcomes.
EHR Implementation Checklist Establish Project Governance
Strong governance is a critical part of any EHR implementation checklist. Clinics should identify key stakeholders across clinical leadership, IT, practice management, and compliance. These stakeholders provide oversight, support decision making, and ensure that the implementation stays aligned with organizational needs. According to the Office of the National Coordinator for Health IT (ONC), governance and leadership engagement are essential for successful EHR adoption and long term system performance.
EHR Implementation Checklist Assign Internal Project Manager
An effective EHR implementation checklist includes assigning a dedicated internal project manager. This individual is responsible for managing timelines, coordinating with vendors, tracking progress, and resolving issues. A strong project manager helps keep the implementation organized and ensures accountability across teams.
EHR Implementation Checklist Define Timeline And Budget
Every EHR implementation checklist should include a clear timeline and budget. Clinics must account for software licensing, hardware upgrades, implementation services, staff training, and workflow redesign. A well defined budget helps prevent unexpected costs and keeps the project on track.
EHR Implementation Checklist Identify System Integrations
An EHR implementation checklist must also include planning for system integrations. Clinics often need to connect the EHR with laboratory systems, imaging systems, billing platforms, patient portals, and health information exchanges. Proper integration planning ensures that data flows smoothly across systems and supports clinical and operational efficiency.
Organizations that need support during this phase often benefit from structured guidance through our EHR Consulting Services, which help align planning, integration strategy, and project execution with implementation goals.

Using an EHR Implementation Checklist for Vendor Selection
Vendor selection is one of the most important steps in an EHR implementation checklist because it directly impacts workflow efficiency, user adoption, and long term system performance. Clinics that follow a structured EHR implementation checklist during vendor selection are better able to evaluate system capabilities, compare vendors, and choose a platform that aligns with clinical and operational needs. A clear and consistent evaluation process reduces risk and helps ensure the selected EHR supports both current workflows and future growth.
Identify Required Features And Capabilities
An effective EHR implementation checklist begins vendor selection by identifying the features and capabilities the clinic needs. These often include specialty specific templates, ePrescribing functionality, clinical decision support tools, and patient portal access. Clearly defining these requirements helps clinics narrow down vendor options and ensures the system supports day to day clinical operations.
Assess Interoperability And Integrations
Interoperability is a critical component of any EHR implementation checklist. Clinics must ensure the system can integrate with laboratory systems, imaging platforms, billing systems, and health information exchanges. Strong interoperability supports better care coordination and reduces manual data entry across systems. The Centers for Medicare and Medicaid Services (CMS) emphasizes interoperability as a key factor in improving care coordination and data exchange across healthcare systems.
Review Security And Compliance
Security and compliance should be a core focus of every EHR implementation checklist during vendor selection. Clinics must confirm that vendors meet HIPAA requirements, provide data encryption, and support role based access controls. Strong security practices help protect patient data and reduce organizational risk.
Workflow Mapping And Data Migration
Workflow mapping and data migration are two of the most critical steps in any EHR implementation checklist. Clinics that do not properly plan these areas often experience delays, staff frustration, and workflow disruption after go live. A structured EHR implementation checklist helps organizations document current processes, identify inefficiencies, and prepare data for accurate transfer into the new system. This phase requires careful coordination between clinical, operational, and technical teams to ensure the system supports real world workflows.
Document And Improve Clinical Workflows
An EHR implementation checklist should begin this phase by documenting current clinical and administrative workflows. This includes patient intake, documentation, order entry, and billing processes. Clinics should review each step to identify inefficiencies, duplicate work, and gaps in communication. Improving workflows before implementation helps ensure the new system supports better efficiency instead of recreating existing problems.
The Agency for Healthcare Research and Quality (AHRQ) highlights workflow analysis as a key step in health IT implementation because it helps organizations align technology with clinical practice and improve patient care outcomes.
Plan and Test Data Migration
Data migration is a core component of any EHR implementation checklist and requires careful planning. Clinics must decide which data to move into the new system, such as patient demographics, medical history, medications, and upcoming appointments. Not all legacy data needs to be migrated, and some information may be archived instead.
Testing is essential to ensure data accuracy. Clinics should conduct test imports to validate field mapping, identify errors, and prevent duplicate records. A structured EHR implementation checklist helps teams complete multiple rounds of testing before go live, which reduces risk and ensures data integrity.

Staff Training And Change Management
Staff training and change management are essential parts of any EHR implementation checklist because system success depends on how well users adopt the new technology. Clinics that invest in structured training are more likely to reduce errors, improve efficiency, and maintain productivity after go live. A well executed EHR implementation checklist ensures that staff understand their roles, feel confident using the system, and are supported throughout the transition.
Training, Adoption, And Ongoing Support
An effective EHR implementation checklist includes identifying super users who can support training and adoption across the organization. These individuals serve as internal experts who help guide staff, answer questions, and provide support during and after go live. Clinics should deliver role based training tailored to providers, nurses, administrative staff, and billing teams so each group understands the workflows relevant to their responsibilities. Practice scenarios help reinforce learning and prepare staff for real world use.
Training should continue after go live to support long term success. A strong EHR implementation checklist includes refresher sessions, access to documentation, and ongoing support resources. The U.S. Department of Health and Human Services (HHS) emphasizes that continued training and user support improve adoption and reduce user related errors. Organizations that prioritize training and change management are more likely to achieve consistent adoption and improved performance.
Using an EHR Implementation Checklist for Go-Live Preparation
Go-live preparation is the final and most critical phase of an EHR implementation checklist because it determines how smoothly the transition will occur. Clinics that follow a structured EHR implementation checklist during this phase are better prepared to manage risk, support staff, and maintain patient care operations. This stage focuses on final testing, operational readiness, and clear communication to ensure all teams are aligned before go live.
Final Testing And Operational Readiness
A complete EHR implementation checklist includes thorough testing of all clinical, administrative, and billing workflows before go live. Clinics should validate patient check in, documentation, order entry, prescribing, and revenue cycle processes to ensure the system functions as expected. End to end testing helps identify issues early and allows teams to make adjustments before the system is fully deployed.
Operational readiness is equally important. Clinics should establish downtime procedures, confirm vendor support availability, and adjust patient schedules to reduce volume during the first days of go live. Clear communication across staff ensures everyone understands their roles and expectations during the transition.
Organizations serving diverse or underserved populations should also consider how go live may impact access to care. Planning for continuity and patient communication supports equitable care delivery during system transitions. For additional insight, explore our whitepaper on advancing health equity in underserved communities, which highlights strategies for maintaining access and improving outcomes during operational change.
Using an EHR Implementation Checklist for Post-Implementation Optimization
Post-implementation optimization is a critical phase of any EHR implementation checklist because the work does not end at go live. Clinics that continue to refine workflows, monitor performance, and support users are more likely to achieve long term success. A structured EHR implementation checklist helps organizations identify improvement areas, increase efficiency, and ensure the system continues to meet clinical and operational needs.
Monitor Adoption And Workflow Performance
An effective EHR implementation checklist includes ongoing monitoring of user adoption and workflow performance. Clinics should track documentation time, template usage, and staff feedback to identify challenges and areas for improvement. Regular review of workflows helps ensure the system supports efficient and consistent patient care.
Evaluate Financial And Operational Impact
A complete EHR implementation checklist should also include evaluation of financial and operational performance after go live. Clinics should monitor claim processing timelines, coding accuracy, and revenue cycle performance to identify any disruptions. Addressing these issues early helps stabilize operations and supports long term financial health.
The Centers for Medicare and Medicaid Services (CMS) emphasizes the importance of accurate documentation and coding in maintaining revenue integrity and compliance in healthcare systems.

Conclusion And Next Steps
A successful EHR implementation checklist requires strong planning, workflow alignment, staff training, and structured go live management. Clinics that follow a clear and organized approach are better positioned to reduce disruption, support adoption, and maintain operational stability.
Many organizations benefit from experienced support during implementation to help manage complexity and ensure long term success. If you are preparing for an EHR implementation, contact our team to learn how we can support your organization through every phase of the process.
Ready to Talk?
Further Reading
-
John Lynch & Associates: NextGen EHR Tips And Tricks To Boost Patient Outcomes
Practical strategies for improving EHR usability, enhancing clinical workflows, and driving better patient outcomes after go live. -
John Lynch & Associates: Advancing Health Equity In Underserved Communities
A strategic whitepaper outlining approaches to maintaining access to care and improving outcomes during operational and technology transitions. -
John Lynch & Associates: EHR Consulting Services
An overview of structured support for EHR implementation, including planning, workflow design, vendor coordination, and go live management. -
Office of the National Coordinator for Health IT (ONC): Health IT Implementation Resources
Guidance on EHR adoption, interoperability, and best practices for aligning technology with clinical workflows. -
Centers for Medicare and Medicaid Services (CMS): Health IT And EHR Programs
Resources on compliance, interoperability, and the role of EHR systems in improving care quality and reporting. -
Agency for Healthcare Research and Quality (AHRQ): Health IT And Workflow Resources
Research and tools focused on workflow analysis, patient safety, and effective health IT implementation. -
U.S. Department of Health and Human Services (HHS): Health Information Technology Resources
Information on health IT adoption, training, and strategies to improve system use and patient care outcomes.
Related Articles

Compliance Audit Checklist: Identify Risks Before an Audit

How to Build an EHR Training Plan That Reduces Go-Live Risk and Accelerates Adoption

